Seniors and Venous Disease
George Burns, that wise philosopher, said it best: "You can't help getting older, but you don't have to get old." There's no denying biology, but when a patient enters his or her golden years, attitude and lifestyle become more relevant to good health than ever.
Dr. Bruce Bates, D.O., FACOFP, CMD has been practicing medicine since 1975. He is the former Associate Dean for Clinical Services at the University Of New England College of Osteopathic Medicine and was the first-ever Chair of the Department of Geriatric Medicine.
Dr. Bates believes that the biggest obstacle when caring for senior patients is ageism—on the part of the doctor and the patient. "What do you expect? I'm old," is a commonly held attitude.
"The acceptance of decreased functionality as normal is a detriment to healthy and successful aging," said Dr. Bates, who was an administrator and part-time physician for MatureCare, a Maine practice specializing in caring for the elderly in live-in facilities or at home.
Veins and aging
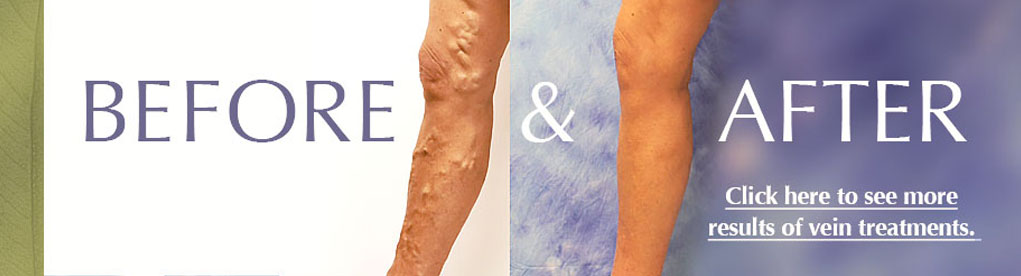
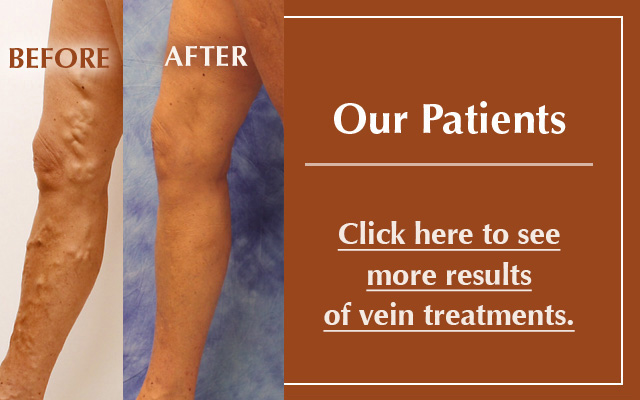
Paying attention to venous health is one aspect of successful aging. Venous insufficiency occurs when healthy veins become damaged and allow the backward flow of blood into the lower extremities. This pooling of blood can lead to a feeling of heaviness, aching, and can cause skin changes, such as spider veins or a brown, woody appearance of the lower legs.
Seniors' veins respond differently to everyday stress compared to that of a younger person's because vein walls are primarily made of collagen. As the body ages, a decrease in the production of collagen causes the veins to become more brittle and the valves more likely to fail, especially in the superficial veins. Thus, there is a higher incidence of varicose veins in the elderly population.
Additionally, the skin begins to lose its elasticity and doesn't respond to stress the way it once did. And because skin is the "end organ" of venous disease, ulcers and bleeding varicosities can occur as a result of damaged veins.
Many seniors think varicose veins and venous stasis ulcers are a normal part of aging, but what they may not know is that they need not suffer with symptoms. Even those who experience an aching or heaviness in their legs can receive treatment and relief. Treating the symptoms also arrests the progression of their disease.
One barrier to treatment is that, in the past, patients' options were limited. "Vein stripping" was the go-to procedure for many years. Treatment of venous disease today, however, is vastly different. Breakthroughs in phlebology and new approaches to treatment involve less time and less pain, and they are overwhelmingly successful over the long term when performed by an experienced specialist. The risk-benefit ratio makes vein treatment an ideal option for seniors.
A trained phlebologist will locate and treat a vein problem at its source, leaving no skin openings other than that of a typical IV access site. Considering the patient's overall health prior to treatment is essential. As with any senior patient, taking into account a patient's comorbidities is one of the most important aspects of venous care.
Common problems and solutions
As discussed earlier, varicose veins are a frequent problem for older patients. Deep vein thrombosis (DVT) is also quite common. DVT occurs when a blood clot forms in one of the large veins—usually one of the lower limbs, such as the thigh or calf—leading to either partially or completely blocked venous return.
The incidence of DVT is higher in older people because of something called Virchow's triad: 1) endothelium damage, including trauma to any blood vessel due to surgery, or even bumping into something, 2) stasis, a decreased blood flow due to immobility, and 3) hypercoaguability, an abnormal tendency toward blood clotting, due to heredity, acquired medical condition or even concurrent medications.
Physicians should consider recommending that their senior patients visit a phlebologist for a superficial venous evaluation, prior to elective surgeries, especially hip or knee replacement. This step will help the patient learn the risks and decrease the chances of developing DVT.
Additionally, seniors tend to be less active because of other medical conditions, such as arthritis or a respiratory issue that makes them less likely to walk or exercise. Walking causes the rhythmic contraction of calf muscles and, like a pump, forces all the blood into the deep veins and helps promote blood flow to the heart. Patients may not realize that walking just 30 minutes a day, even in three-minute increments, can improve vein (and overall) health.
Compression therapy is common in venous care, especially for seniors, but misapprehensions about compression stockings can sometimes be an obstacle. It's important to make the distinction between graduated compression stockings and T.E.D. hose; they should never be used interchangeably.
Senior patients may have tried compression stockings years ago, before newer designs and donning devices were available. They may not know that there are now compression stockings on the market that are much more tolerable. There are even groups that send people to patients' home to assist with putting stockings on.
Historically, seniors would often opt for conservative methods, such as long-term compression, elevation and regular exercise. However, when a senior is educated on new treatment options, there is often a willingness to explore definitive therapy, such as intervention.
Follow up is extremely important. No matter what the problem is, following through with long-term care for the patient is critical when dealing with chronic diseases like venous insufficiency.
Although seniors have a 50% greater chance of suffering from vein disease, they have the same success with modern treatment options as anyone else. Modern techniques, such as endovenous ablation or ultrasound-guided sclerotherapy, are the most effective solutions for the majority of vein problems.
They are minimally invasive, highly successful, and are not reserved for the young.
Goals and expectations
Seniors are a diverse population in terms of their baseline health and their expectations. Someone who is 85 years old with end-stage dementia is obviously going to merit different treatment than another 85-year-old old who plays tennis three times a week. One patient might have as his goal to get out of compression stockings, whereas another might be thrilled to hear that her treatment is only compression stockings.
Knowing and understanding the individual patient is paramount. Dr. Bates' talks with each patient on a one-to-one basis, setting realistic, achievable goals for ability, rather than emphasizing disability. In order to develop a strategy to attain those goals, Dr. Bates stresses a team approach: primary care physicians, nurses, occupational therapists, specialists, and even spouses or significant others all play a role in the patient's support system. He says that ideally, the "captain of the ship" is the primary care physician.
Although Dr. Bates has dealt with the 5% of the elderly population that is frail enough to require round-the-clock care, he believes that we should pay as much attention to the 95% who are currently ambulatory and healthy.
"They're the ones we need to get to, before the cramping, achiness and illness," said Dr. Bates. "If we would but look, and ask, we can identify them before they require expensive treatment—not just in dollars, but also in terms of lifestyle, comfort, self-worth, mobility."
Thinking about aging in a functional, positive way, rather than a declining, dysfunctional way leads to one conclusion: prevention. In venous care, early, high-quality treatment can be the best form of prevention.
This article was featured in Vein Health News, a publication founded by Dr. Cindy Asbjornsen to educate medical professionals and patients about vein health.

Dr. Asbjornsen is the Editorial Director for Vein Health News, Maine's vein magazine for primary care physicians. Read the Latest Issue and Subscribe to Vein Health News.
![]() Do I have Venous Disease?
Do I have Venous Disease?
Millions of people across the United States experience its symptoms. Find out more by asking yourself these 12 questions.
 Request an Appointment
Request an Appointment
Ready to take the next step towards understanding your vein health and the available treatment options? Click here to request an appointment.